Featured new articles related to intranasal drug delivery:
October - December 2013
___________________________________
Andolfatto, G., E. Willman, et al. (2013). "Intranasal Ketamine for
Analgesia in the Emergency Department: A Prospective Observational
Series." Acad Emerg Med 20(10):
1050-1054.
OBJECTIVES: The objective was to examine the
feasibility, effectiveness, and adverse effect profile of intranasal
ketamine for analgesia in emergency department (ED) patients. METHODS:
This was a prospective observational study examining a convenience
sample of patients aged older than 6 years experiencing moderate or
severe pain, defined as a visual analog scale (VAS) score of 50 mm or
greater. Patients received 0.5 to 0.75 mg/kg intranasal ketamine. Pain
scores were recorded on a standard 100-mm VAS by trained investigators
at baseline, then every 5 minutes for 30 minutes, and then every 10
minutes for an additional 30 minutes. The primary outcome was the number
and proportion of patients experiencing clinically significant
reductions in VAS pain scores, defined as VAS reductions of 13 mm or
more, within 30 minutes. Secondary outcomes included the median
reduction in VAS, the median time required to achieve a 13 mm reduction
in VAS, vital sign changes, and adverse events. Continuous data are
reported with medians and interquartile ranges (IQRs). The Wilcoxon
signed-ranks test was used to assess changes in VAS scores. Adverse
effects are reported with proportions and 95% confidence intervals
(CIs). RESULTS: Forty patients were enrolled with a median age of 47
years (IQR = 36 to 57 years; range = 11 to 79 years) for primarily
orthopedic injuries. A reduction in VAS of 13 mm or more within 30
minutes was achieved in 35 patients (88%). The median change in VAS at
30 minutes was 34 mm (44%). Median time required to achieve a 13 mm VAS
reduction was 9.5 minutes (IQR = 5 to 13 minutes; range = 5 to 25
minutes). No serious adverse effects occurred. Minor adverse effects
included dizziness (21 patients, 53%; 95% CI = 38% to 67%), feeling of
unreality (14 patients, 35%; 95% CI = 22% to 50%), nausea (four
patients, 10%; 95% CI = 4% to 23%), mood change (three patients, 8%; 95%
CI = 3% to 20%), and changes in hearing (one patient, 3%; 95% CI = 0% to
13%). All adverse effects were transient and none required intervention.
There were no changes in vital signs requiring clinical intervention.
CONCLUSIONS: Intranasal ketamine reduced VAS pain scores to a clinically
significant degree in 88% of ED patients in this series. Adverse effects
were minor and transient. Intranasal ketamine may have a role in the
provision of effective, expeditious analgesia to ED patients.
Web site Editorial comments:
Here is another IN ketamine article evaluating this drugs effectiveness as an analgesic (not as a sedative). This is the first study on this topic in adults in an emergency room (Johansson also recently published a study for use in the prehospital setting). The authors found this treatment (0.5 to 0.75 mg/kg of intranasal ketamine) to have a clinically significant impact on pain reduction in 88% of patients. The mean pain score reduction was 34 mm on a 100 mm scale. The median time to onset was just under 10 minutes. Side effects were minor. This suggests a potential use for IN ketamine in the setting of acute severe pain in adults – cheap, fast, relatively effective with minimal side effects. Personally I think they used a dose that is a bit low when compared to other studies that used 1 mg/kg, but since this is a relatively new concept, picking a proper first dose can be difficult. Also IN sufentanil may be more compelling for pain control in adults based on recent data showing pain score reductions of 57 mm at 30 minutes (Steenblick). However, there are rare issues with mild respiratory depression using IN sufentanil (especially in the elderly) so it is definitely of higher risk that IN ketamine. The authors specifically mention this issue as the real advantage of IN ketamine – no need for monitoring in a busy or overcrowded department. Perhaps based on the situation either drug would be selected or at times a combination. Hopefully these questions and the ideal dose will be sorted out with further research studies.
Pubmed link: http://www.ncbi.nlm.nih.gov/pubmed/24127709
___________________________________
Gracia, M. R., L. C. Hortelano, et al. (2013). "Intoxicación
accidental por
fentanilo intranasal." Anales de Pediatria
In press.
The abstract is not available as this was a letter to the editor written in Spanish. Instead we just review the issue in the editorial comments below.
Web site Editorial comments:
This website had previously stated that there
are no reports of significant adverse events related to IN fentanyl, but
has also stated that sufentanil which is 8-10 times more potent can
cause respiratory depression. These statements have been based on many
hundreds to thousands of uses of IN fentanyl in pediatric practice using
generic fentanyl at concentrations of 50 mcg per ml. Recently, nasal
fentanyl has been put on the market as a hospice and chronic pain
medication for use in adults.
These drugs
are extremely highly concentrated – to doses as high several thousand
micrograms per ml so that a single 1/10 ml spray may contain hundreds of
micrograms of drug. In this situation, overdose is possible and likely
in children due to the very high plasma levels that will be obtained
despite the slower absorption of the nasal drug and the delayed peak
activity. Gracia points this fact out by reporting the respiratory
depression and desaturation that occurred when two young boys got a hold
of an adult dispenser of this medication and accidentally administered
doses to their noses of 400 mcg. Both boys requiring naloxone for
recovery – one IN, the other IM.
In our
practice we are quite happy with the safety and efficacy (and low cost)
of IN fentanyl in the generic formulation (50 mcg/ml). Our experience
for over a decade using this medication for acute fractures, burns and
other acute painful issues in pediatrics is excellent. We do use IN
sufentanil (also at 50 mcg/ml) in adults and do find some mild
respiratory depression primarily in the elderly with this more potent
opiate (saturations in the 88-90% range at our altitude of 4500 feet –
1500 meters) which we are comfortable with observing until it wears off.
I do not see the need in acute care for these more concentrated
formulations given the efficacy and safety profiles of the lower
concentrations.
PDF: Free in press article PDF (click here)
Pubmed link: http://www.ncbi.nlm.nih.gov/pubmed/23684172
___________________________________
Mitra, S., S. Kazal, et al. (2013). "Intranasal clonidine vs midazolam
as premedication in children: A randomized controlled trial." Indian
Pediatr (In press).
Objectives: To compare anxiolysis produced by intranasal clonidine with intranasal midazolam as premedication in children undergoing surgery. Design: Double-blind randomized controlled study. Setting: Tertiary-care hospital, July 2009 to June 2010. Patients: 60 American Society of Anesthesiologists physical status I-II surgical patients 1-10y old. Intervention: The participants were randomly allocated to two groups to receive either intranasal clonidine 4mcg/kg (Group I) or intranasal midazolam 0.3mg/kg (Group II). Outcome measures: The primary outcome measure was proportions of patients with satisfactory anxiolysis at 30 min after drug administration. Secondary outcome measures included satisfactory mask acceptance, times of onset of sedation and anxiolysis, drug acceptance, level of sedation, wake-up score and side effects. Results: All children achieved satisfactory anxiolysis at 30 min. Group I fared significantly better than Group-II on mask acceptance (100% in Group I vs. 80% in Group II; P=0.024), drug acceptance (93% vs. 13%; P<0.001) and proportion of patients with satisfactory wake-up scores (100% vs. 53%; P<0.001). Group II patients had significantly faster onset of sedation (median 10 min vs. 15 min; P<0.05) but not that of anxiolysis compared to Group-I (median 10 min for both groups; P>0.05). Side effects were significantly more frequent in Group II. Conclusions: Though intranasal midazolam produced faster sedation, both the drugs produced satisfactory anxiolysis at 30 min. Mask acceptance and several other secondary outcomes were significantly better with intranasal clonidine.
Web site Editorial comments:
This study randomized 60 children to either IN
midazolam 0.3 mg/kg (5 mg/ml generic solution) or IN clonidine 4 mcg/kg
(150 mcg/ml solution) plus 0.6 mg of atropine. The primary outcome was
adequate sedation at 30 minutes. Secondary outcomes were crying after
drug delivery and mask acceptance in the operating suite. All 60
patients (30 per group) achieved adequate sedation by 30 minutes though
it was faster onset (20 minutes) with midazolam. The clonidine group had
better acceptance of the drug with less crying and they had better mask
acceptance and calmer awakening. The authors conclude: “intranasal
clonidine has been shown to produce comparable level of sedation as
effective anxiolysis as nasal midazolam after 30 min, but with a better
mask acceptance and recovery profile.”
There are some quite serious flaws in the study
design which in 2013 are really not excusable given the easy access to
data via the internet and the huge database that is 20 years old showing
that midazolam sedation requires a dose of more than 0.3 mg/kg nasally.
Another flaw is that the well known downside of burning upon application
that can be mitigated by combining it with a topical anesthetic.
Furthermore they delivered the drug in a recumbent position with a
dropped syringe – which tends to lead to a lot of runoff into the
hypopharynx (i.e. oral drug) and loss of any true nasal absorption
further limiting the drugs effectiveness. Never the less, the study is
interesting in that someone finally did a moderate sized trial on a very
inexpensive Alpha-2 agonist – Clonidine – and showed it is very
effective at preoperative anxiolysis and sedation without the issue of
burning upon application. This has been hinted at by prior case reports
of intranasal clonidine and by many trials of a more expensive alpha-2
agonist dexmedetomidine. In the era of health care cost concerns, it
might be time to further investigate this very inexpensive sedation
option – nasal clonidine, delivered by an atomizer. Good efficacy and
safety data on this medication might be compelling enough to convince
many clinicians to switch from midazolam to clonidine or to actually
even consider nasal medication for sedation and anxiolysis for minor
procedures.
Internet link for free article: http://www.indianpediatrics.net/Epub05092013/RP-00299.pdf
___________________________________
Sharma, R. and R. Harish (2013).
"Comparative study of the efficacy of intranasal midazolam vs
intravenous midazolam in convulsing neonates and children." RRJMHS
2(4): 54-57.
To
compare the
efficacy of
intranasal midazolam
in relation
to intravenous midazolam for control of seizures. To observe
variability if any amongst
the two
groups in
terms of
heart rate,
respiratory rate,
blood pressure and
oxygen saturation.
A Prospective
Randomized study
conducted on
100 patients
of 0-19
years of
age hospitalized
in emergency ward and NICU in a convulsing state. They
were divided into two groups. GP-I was given intranasal midazolam
@ 0.3 mg/ kg and GP-II was given intravenous midazolam @ 0.3 mg/ kg.
Outcome was measured in
terms of:
Time taken
from physician
contact to
drug administration.
Time taken from drug administration to cessation of seizures.
Mean time from
physician contact
to drug
administration was
significantly shorter
with intranasal
midazolam as
compared to
intravenous midazolam
viz [ 0.40+
0.10min vs
1.06+0.40+min) [p<
0.05 ].Mean
time from
drug administration
to cessation of
seizures was
comparable in
both the groups
1.0 +
0.31 min
and 1.0+0.32
min (p>
0.05). However
this difference was
statistically
insignificant. The
readings for
oxygen saturation and
vital parameters
did not
show a
statistically
significant difference
amongst the
groups. Seizure
control
was more
prompt with
intranasal midazolam
as compared
to intravenous
midazolam. As
time needed for
drug administration
was lesser.
Intranasal midazolam
is a rapid,
efficacious, easy to administer and socially more acceptable route of
drug administration. It can
be used not only in hospital setting but also for home management of
seizures after proper instructions to parents.
Web site Editorial comments:
Here is our 4th
or 5th prospective randomized trial comparing intranasal benzodiazepines
to the gold standard intravenous benzodiazepines for the treatment of
status epilepticus. As in every other prospective trial on the topic the
two treatment are equivalent in terms of efficacy: In this study both
were successful at stopping seizures 94% of the time with a single dose.
The intranasal route was also slightly faster likely due to the delays
associated with IV line establishment. Unique to this study was the
inclusion of neonates: There were 7 neonates in this study and an
additional
26 children under the age of 1 year.
Internet link to free article: (click for link to free article)
___________________________________
Title:
Abstract
Web site Editorial comments:
Pubmed link:
___________________________________
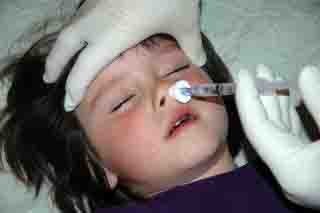 Therapeutic
Intranasal Drug Delivery
Therapeutic
Intranasal Drug Delivery