Intranasal Sedation overview:
Topic summary:
Nasal delivery of sedatives is one of the original uses for nasal medications in clinical practice. Many studies exist from the 1980's and 90's using midazolam in preoperative setting to sedate children. Since that time a growing body of literature demonstrates efficacy of this concept in the pediatric operating room but also in very diverse medical settings where non-injectable sedation is attractive: Dental patients (needle phobic, developmentally delayed, pediatric), almost any pediatric procedure, adult minor procedures usually in combination with a nasal opiate (abscess drainage, burn care, chest tubes, etc), anxiolysis for cross sectional imaging, agitated delirium, and more. It is an attractive form of sedation in settings where patients could be helped with mild to moderated sedation, yet do not have any IV access. There is extensive literature on this topic (reviewed on this website) showing IN sedation done properly with the right drugs and the right doses enhance the clinicians ability to care for patients in a very cost effective manner. The technique can be titrated and if benzodiazepines are used, the drugs can be reversed by intranasal flumazanil if a problem arises. The most extensively studied intranasal medications are midazolam and dexmedetomidine. Other medications that have been studied include sufentanil, lorazepam and ketamine. This overview section provides a quick look at the topic and provides dosing and protocols. Digging deeper behind this page is an extensive review the literature with supporting references (Click here to skip the overview below and to go directly to the deeper discussion).
Key Concepts regarding delivery of any nasal medication to the systemic circulation and brain
Use the right dose!
- Nasal medication doses are NOT equivalent to IV dosing. Using an IV dose will usually fail. (Read about bioavailability in the Overview page)
- A general rule of thumb is you will need twice the IV dose (often times more). For midazolam sedation you will need 4-5 times the IV dose. This website provides extensive literature to support the doses recommended. Read those studies to assist you will deciding the dose you feel is appropriate for the clinical situation.
- Respiratory depression is rarely a concern with nasally delivered generic concentrations of drugs - so use the right dose. Click here for a brief but more in depth discussion on this concept.
Minimize volume, maximize concentration of the drug
- Use the most concentrated (potent) available formulation
appropriate for the task
- eg: IN Midazolam should be done using 5 mg/ml concentration, not the 1 mg/ml concentration.
- Do NOT dilute the drug
- 0.2 to 0.3 ml per nostril is an ideal volume in the clinical setting - good coverage but low risk of significant drug loss from delivery error. We push it up to 1 ml/nostril if needed realizing there will be some drug loss.
Large volumes are lost into the pharynx or out the nostril.
Maximize total absorptive surface area
- Use BOTH nostrils for volumes over 0.3 ml. This doubles the absorptive surface area and reduces runoff.
- ABOUT half per nostril is clinically adequate - do not worry about being exact.
Use a delivery system that maximizes mucosal surface area coverage and minimizes loss to the environment and runoff
- Droppers work in research using cooperative patients who hold still for many minutes. They tend to be less effective in clinical trials.
- Atomization (not nebulization over minutes) allows immediate delivery of all the drug directly to the mucosa in a broad area of coverage with little loss to the environment. This improves clinical effect and does not require a cooperative patient.
- Account for device dead space in your dosing calculations especially for children or small drug volumes.
Be thoughtful about anatomic issues and head positioning to enhance delivery
- If the patient is cooperative - Occiput/crown down (neck extended in sitting position) delivers more drug higher onto the turbinate's to enhance absorption and nose-brain transport.
- Blood and mucous should be suctioned if possible to enhance mucosal coverage.
- Use of vasoconstrictors might reduce drug absorption (cocaine, epinephrine, oxymetazoline, phenyephrine)
Key Concepts related to nasally delivered sedatives
Dosing: The dose for nasal drug is higher than IV drug. This occurs because not all the drug is absorbed and that which is absorbed takes longer and peaks at lower levels in the blood stream. See below for doses supported by the literature. Failure to use the adequate dose will likely lead to failure to sedate
Respiratory depression: Generic midazolam delivered intranasally does not lead to respiratory depression. Click here for a brief but more in depth discussion on this concept.
Nasal burning: Midazolam burns upon application. This can be reduced or eliminated by using topical lidocaine simultaneously or in advance. Be aware of this side effect and warn the parents that the child will cry, then become sedated in about 5 minutes, peaking at 15-20 and wearing off by 30.
Anxiolysis vs sedation: Midazolam does not provide very deep sedation and the length of sedation is brief. Deeper sedation is possible if combined with an opiate or if dexmedetomidine is used (slower onset, deeper, longer lasting).
Titration: Repeated doses given every 10-15 minutes for the benzodiazepines can lead to more titrated effect.
Reversal: A very small amount of literature exists showing that benzodiazepine induced respiratory depression can be reversed with nasal flumazanil.
Dosing information and delivery protocol
- Midazolam - 0.4 to 0.5 mg/kg
- Sufentanil - 1.0 to 1.5 mcg/kg - may cause respiratory depression in elderly, less likely in children (who metabolize it faster)
- Dexmedetomidine - 2 to 3 mcg/kg
- Ketamine - 10 mg/kg (Still being studied, probably better IN for pain control at 1 mg/kg dose)
Protocol for intranasal midazolam, sufentanil and dexmedetomidine, ketamine (click here)
Commonly used generic intranasal medications - single page dosing summary (click here)
In Depth literature review, discussion, bibliography (Click here)
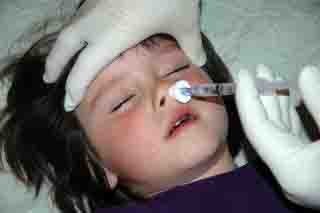 Therapeutic
Intranasal Drug Delivery
Therapeutic
Intranasal Drug Delivery