"Off Label" medication delivery
Table of contents
Medical and legal issues surrounding "Off Label" drug and device use (click here)
Impact of Off label use on clinical practice (click here)
Medical and legal issues surrounding "Off Label" drug and device use
The Food and Drug
Administration (FDA) approves drugs for specific intended uses (clinical
indications) based on the results of extensive clinical trials and a
lengthy drug development and approval process.
When a drug is approved for human use, it is approved for
specific doses, specific age groups and specific routes of
administration. Current
estimates are that a new chemical entity (NCE) takes approximately 15
years at a total cost of up to $650 million to reach the market. It is
virtually impossible for a new drug to get approved for all indications,
ages and dosage forms. However once the product is marketed, creative
clinicians often start exploring new uses and new indications in an
attempt to help their patients. These investigations and “off-label” use
are more common in disease states that are uncommon and where there is
little financial incentive for the manufacturer to pursue additional
indications.[1]
Because of this huge time and cost investment, pharmaceutical companies do not attempt to gain approval for minor indications or routes of administration. Clinicians are allowed (expected) to use their professional judgment as to the use and administration of the drug if not described in the approved labeling. However, some clinicians misinterpret “off-label” use of medications as an illegal or medically dangerous practice. This is not the case. A nice review on the legal aspects of this topic was published in the Journal of Medical Toxicology in September 2006.[2](click here for full article) Because many (most?) antidotes used in toxicology are used for off label indications (which will remain off label due to rare need and no financial incentive to get approval) the toxicologists who published this review article have a special interest in the topic. The author of this article quotes several important statements by medical and legal entities in the United states including the U.S. supreme court and the FDA: The U.S. supreme court has ruled that the “off-label usage of medical devices is an accepted and necessary corollary of the FDA’s mission”… and that health care practitioners can “prescribe or administer any legally marketed device to a patient” without limitation or interference. This opinion is supported by the Center for Drug Evaluation and Research: “Any approved product may be used by a licensed practitioner for uses other than those stated in the product label.” Finally, the FDA itself supports this practice, recognizing that “off-label use is a well-established principle that has allowed doctors to discover new and beneficial uses” for previously approved drugs.
While it is clear that the regulatory and legal entities in the United States support or at the least do not interfere with off-label drug and device use, this does not imply that off-label use should not be carefully evaluated. All off-label use of medications (and on-label use) should be done with careful insight and understanding of the risk benefit ratio. The primary question that should be asked before using any medication, including an on or off-label indication, is whether there is quality evidence supporting the use and if the clinical benefit is expected to outweigh the risk. This concept is eloquently summarized by an Australian committee that developed consensus guideline for off-label medications:[3] “Routine off-label use can be justified if there is high-quality evidence supporting efficacy or effectiveness, and sufficient evidence about the medicine’s safety profile to suggest and overall reasonable benefit –risk for a given clinical context”Impact of "Off Label" use on clinical practice
Off label
medication use is estimated to occur in 7.5 to 40% of adults usage, and
as high as 80% of pediatric inpatient usage.[3-7] This is probably due
to a combination of new evidence supporting off label use, failure of
the manufacturer to pursue new indications due the insufficient
incentives (i.e. no profit in it) and simply using medications without
supporting evidence.[3]
Once creative
investigators have determined the viability of a new indication,
industry may become involved and take the idea to the next level – i.e.
spend the vast sums of money required to prove adequate safety / risk
profiles so they can legally market the concept to the broad medical
market. However, industry will not undertake this risk and expense if
they do not believe they can obtain a reasonable return on their initial
investment. For this reason many well established medical therapies are
never formally approved for use by regulatory agencies. Obvious examples
of commonly used “off-label” medications are most medications provided
to children and pregnant women, toxicology antidotes, H-2 blockers for
hives, ophthalmologic
drug indications and advanced cardiac life-support medication
guidelines.[1, 2, 4, 7] In fact, approximately 80% of medications used
in hospitalized pediatric patients have no formal FDA or European agency
approved use in children.[4, 7] These medications have already been
approved for adult use and the pharmaceutical companies do not see the
need to spend significant additional money on obtaining formal pediatric
indications – so they never are obtained. ACLS guidelines recommend
endotracheal drug administration of epinephrine, atropine and lidocaine,
yet these drugs have never been approved for transmucosal pulmonary
medication delivery. Numerous additional examples exist for psychiatric
medications, clotting medications, H2 blockers for allergies, etc.
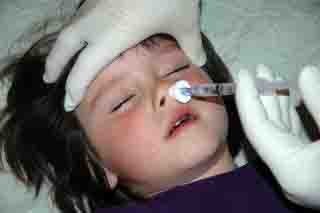
Intranasal
medication delivery falls into a similar situation. Intranasal drug
delivery is a novel concept that only recently has seen randomized
controlled trials to confirm their effectiveness in selected clinical
situations such as pediatric seizure control and pain control.
These studies were conducted using generic medications so the
pharmaceutical companies will have little interest in spending the money
to obtain formal regulatory agency approval for a generic medication.
However, given the literature to support effective and safe use of these
off-label medications (data is provided throughout this web site), it is
reasonable for clinicians to adopt these practices in the appropriate
clinical situations.
In the mean time, now that they see a potential for profit, the
pharmaceutical industry is aggressively developing modified intra-nasal
formulations of these generic medications so they can be patented.
We should soon see trade-name, patent protected formulations of
these generic medications approved and available on the market.
Clinicians will then be able to choose between these products and the
far less expensive but perhaps slightly inferior (or not) generic substitutes.
(Interestingly, many of the drugs discussed on this web site are now
available as generics prepackaged in prefilled syringes -
Carpuject - so this syringe can simply be
attached to an atomizer and delivered into the nose with total costs
probably in the $5 to $7 dollar range for drug and supplies).
There may or may not be compelling reasons to pay the extra price for
the patented products depending on literature comparing them to generic
substitutes. Only time will tell.
United Kingdom document on off label use stating similar regulations as in the United States - Using licensed drugs for unlicensed purposes (click here)
Bibliography (Click here for abstracts)
1. Khamar, B.,
Off-label use of medicines:
medical research and medical practice. Indian J Ophthalmol, 2007.
55(6): p. 411-2.
2. Tomaszewski, C.,
Off-label: just what the doctor
ordered. J Med Toxicol, 2006.
2(3): p. 87-8.
3. Gazarian, M., et al.,
Off-label use of medicines:
consensus recommendations for evaluating appropriateness. Med J Aust,
2006. 185(10): p. 544-8.
4. Shah, S.S., et al.,
Off-label drug use in hospitalized
children. Arch Pediatr Adolesc Med, 2007.
161(3): p. 282-90.
5. Rayburn, W.F. and K.C.
Farmer, Off-label prescribing during pregnancy. Obstet Gynecol Clin North
Am, 1997. 24(3): p. 471-8.
6. Brosgart, C.L., et al.,
Off-label drug use in human
immunodeficiency virus disease. J Acquir Immune Defic Syndr Hum
Retrovirol, 1996. 12(1): p.
56-62.
7. Conroy, S., et al.,
Survey of unlicensed and off label
drug use in paediatric wards in European countries. European Network for
Drug Investigation in Children. Bmj, 2000.
320(7227): p. 79-82.
 Therapeutic
Intranasal Drug Delivery
Therapeutic
Intranasal Drug Delivery