Epistaxis Therapy (Bloody Nose)
Table of Contents:
Introduction to epistaxis therapy with topical drugs (click here)
Literature overview and discussion (click here)
Personal insights from experienced clinicians (click here)
Treatment protocol (click here)
Introduction
Patients with acute anterior epistaxis (bloody nose) frequently visit the emergency department when they are unable to control or stop their nosebleed. Traditional care of these patients includes a stepwise process initially using topical anesthetics and vasoconstrictors such as 4% cocaine alone or lidocaine plus epinephrine. Once the bleeding is controlled and the nasal mucosa can be visualized cautery and nasal packing are often provided.[1] If patients require treatment beyond simple topical medication application they consume significantly more emergency room or clinic resources in terms of materials, physician time, ENT consultations and even operative intervention.[2, 3] In addition, patients requiring home nasal packing are uncomfortable and they suffer an increased risk of sinus infection, hypoxia, hypercapnia and myocardial ischemia.[1, 3, 4] Reducing the need to progress beyond simple topical medication application would simplify care of these patients, allow many patients to self treat at home for future similar spells, shorten their emergency room or clinic length of stay, reduce costs and possibly reduce morbidity.
 The
optimal topical medication for the treatment of epistaxis has not been
extensively investigated. Options include topical vasoconstrictors,
which are inexpensive, and topical clotting factors such as thrombin,
which are more expensive. Topical vasoconstrictor options include
cocaine, phenylephrine and oxymetazoline. Unfortunately, topical
epinephrine (usually combined with lidocaine for anesthesia) is
relatively ineffective.[5] Topical cocaine is more effective than
lidocaine/epinephrine but presents problems due to the fact that it is a
controlled substance and its cost has skyrocketed in the last 2
decades.[6] Furthermore, the cardiovascular stimulation that can occur
with cocaine might be a problem in the elderly as the very young.
Phenylephrine can also cause substantial cardiovascular
stimulation when it is absorbed systemically.[7-9] Due to the risk of
cardiovascular complications, routine cocaine or phenylephrine use for
epistaxis may not be warranted.
The
optimal topical medication for the treatment of epistaxis has not been
extensively investigated. Options include topical vasoconstrictors,
which are inexpensive, and topical clotting factors such as thrombin,
which are more expensive. Topical vasoconstrictor options include
cocaine, phenylephrine and oxymetazoline. Unfortunately, topical
epinephrine (usually combined with lidocaine for anesthesia) is
relatively ineffective.[5] Topical cocaine is more effective than
lidocaine/epinephrine but presents problems due to the fact that it is a
controlled substance and its cost has skyrocketed in the last 2
decades.[6] Furthermore, the cardiovascular stimulation that can occur
with cocaine might be a problem in the elderly as the very young.
Phenylephrine can also cause substantial cardiovascular
stimulation when it is absorbed systemically.[7-9] Due to the risk of
cardiovascular complications, routine cocaine or phenylephrine use for
epistaxis may not be warranted.
 Topical
oxymetazoline (generic Afrin), however, works very well for the
treatment of epistaxis. Due to its dramatic vasoconstrictive effects
oxymetazoline provides excellent control of nasal bleeding while
simultaneously preventing its own systemic absorption, thereby
preventing much cardiovascular effect. Perhaps best of all it can be
purchased over-the-counter and used by the lay public to self treat
bloody noses – often preventing the need to visit the doctor. A number
of prospective studies have found oxymetazoline to be superior to many
of the other vasoconstrictors in preventing bleeding during nasal
procedures.[5, 10, 11]
Several retrospective investigations have also found
oxymetazoline effective in for the emergent treatment of moderate to
severe epistaxis.[12,13]
Topical
oxymetazoline (generic Afrin), however, works very well for the
treatment of epistaxis. Due to its dramatic vasoconstrictive effects
oxymetazoline provides excellent control of nasal bleeding while
simultaneously preventing its own systemic absorption, thereby
preventing much cardiovascular effect. Perhaps best of all it can be
purchased over-the-counter and used by the lay public to self treat
bloody noses – often preventing the need to visit the doctor. A number
of prospective studies have found oxymetazoline to be superior to many
of the other vasoconstrictors in preventing bleeding during nasal
procedures.[5, 10, 11]
Several retrospective investigations have also found
oxymetazoline effective in for the emergent treatment of moderate to
severe epistaxis.[12,13]
Literature overview and discussion
The traditional management for epistaxis has been nasal packing, which is quite effective.[1, 13] This may explain why the literature regarding topical vasoconstrictor therapy alone for the treatment of epistaxis is relatively small. Another explanation may be that many investigators do not feel the topic is worth conducting research studies. Regardless of the reason, only a few published studies exist – several which are reviewed below.
Katz et al prospectively compared topical lidocaine plus epinephrine vs. cocaine vs. oxymetazoline for the prevention of epistaxis in nasotracheal intubation.[5] They found that lidocaine plus epinephrine was only 29% effective, cocaine was 57% effective and oxymetazoline was 86% effective in preventing bleeding during this procedure. The results suggest that the less expensive, lower side effect profile of oxymetazoline made it an effective if not preferred choice for prevention of epistaxis during nasal intubation.
In 1995, Krempl and Noorily reported their experience with oxymetazoline in 60 emergency and clinic patients with acute epistaxis.[13] They found that bleeding resolved in 65% of patients with topical intranasal oxymetazoline alone. Oxymetazoline plus silver nitrate cautery fixed another 18%, leaving only 17% of patients who needed nasal packing or more aggressive care. All patients with controlled bleeding (54 of 60) were sent home with the oxymetazoline spray and instructed to use it three times a day for three days. Only one case returned with recurrent epistaxis (which was easily treated with silver nitrate cautery). The authors conclude that topical intranasal oxymetazoline should be first line therapy for acute epistaxis, and that patients treated thus should be sent home with instructions to continue topical oxymetazoline for several additional days.
Doo and Johnson reported similarly high efficacy for control of posterior epistaxis (a far more serious situation) with topical intranasal oxymetazoline.[12] Of 36 patients presenting for treatment, 27 (75%) had their bleeding controlled with topical oxymetazoline alone. The authors felt these results were compelling enough to suggest an initial pharmacologic treatment of posterior epistaxis with oxymetazoline in an effort to reduce the costs and complications associated with posterior epistaxis packing and surgical ligation.
An interesting case series was reported in 2018 - Heymer et al describe their protocol for epistaxis which routinely includes 2 ml of atomized tranexamic acid, with re-dosage if bleeding occurs.[15]
Interpretation of the literature as it currently exists in 2010- Upsides and downsides:
Epistaxis is a common and messy problem that requires substantial time and resources to treat effectively. Interestingly, a number of authors in the ENT field have noted that the majority of epistaxis can be easily controlled with a simple application of intranasal oxymetazoline (AfrinÒ) followed by a brief period of patient applied pressure.[12, 13] This treatment method eliminates the need, discomfort, expenses and risks of nasal packing and antibiotics, and the patient can take the oxymetazoline home with them and continue treatment for a few days to prevent recurrence. Topical oxymetazoline can also be started by nursing staff upon a patient’s arrival to an ED or clinic - resulting in cessation or slowing of the bleeding before the physician sees the patient. Pretreatment of the nasal mucosa with oxymetazoline is also useful to prevent epistaxis prior to nasal procedures such as intubation, nasopharyngeal airway placement and nasogastric tube placement.[5] All these advantages come with apparently little or no reported risk in terms of drug side effects such as hypertension.
While the data is small (more controlled trials would be helpful), the best current evidence suggests that intranasal oxymetazoline is an excellent first line therapy for epistaxis. Given the large potential benefits and small risks, this treatment should likely be instituted in almost all emergency department and clinic patients with epistaxis. If it fails, there is little downside – cautery, packing and ENT consultation can still be obtained. If it succeeds the patients can be educated, given the medication (or told to buy it over the counter) and discharged with instructions to re-dose their nose two to three times a day for several days in an effort to prevent recurrent bleeding.
Patients who suffer recurrent bloody noses can also institute these treatment concepts at home. By self-treating with a simple protocol (see below – use the bottle as the sprayer) most bleeding can be controlled and stopped without the need to visit a physician.
Avastin for recurrent epistaxis due to hereditary hemorrhagic telangiectasia
Dr. Terence Davidson, an ENT surgeon in California has conducted several small studies and has an ongoing large trial looking at the effectiveness of avastin for treating patients suffering from chronic recurrent nose bleeds due to hereditary hemorrhagic telangiectasia. His data to date show that nasal spray is safer than injection (no risk of septal perforation or necrosis) and effectively stops growth of excessive blood vessels, preventing nose bleeds from recurring.[14]
Tranexamic acid for treatment of epistaxis
Epistaxis can be a messy problem in the ED when traditional packing
methods are used, and it is quite uncomfortable for the patient.
Utilizing an atomizer along with inexpensive medications such as
tranexamic acid and perhaps some oxymetazoline plus external compression
makes the care of these cases much easier and more comfortable.
In 2013 a novel study
was published by Zahed et al where they discussed their results from an
RCT comparing topical tranexamic acid (TXA) to traditional nasal
packing.(16) The results were very impressive: Control of bleeding in 10
minutes 71% vs. 31%, Discharge in less than 2 hours 95% vs. 6%,
rebleeding 5% vs. 11%, patient satisfaction much higher for TXA.
These results were not a fluke, following this impressive
publication multiple additional studies have been published, most which
have shown impressive results when compared to either nasal packing or
nasal vasoconstrictors.(17-29)This is a
great new treatment option for epistaxis and I suspect it will be
rapidly adopted given its low cost and demonstrated efficacy for a
sometimes difficult situation.
Personal insights from experienced clinicians
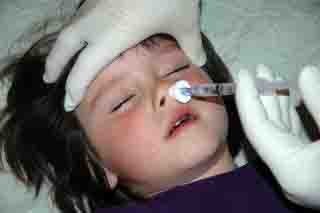
At the Everest base camp medical clinic, conditions are cold and hostile, nearly every case is urgent, and routine treatment we rely on in urban hospital environments is sometimes impossible to carry out. Having the ability to administer medications intranasally, obviating the need for IV access (and thawing out of our IV fluids!) can be not only an easier and timelier solution, but downright lifesaving! In our recent 2008 season, our staff had the opportunity to treat a brisk nosebleed patient by administering intranasal oxymetazoline and lidocaine to facilitate insertion of a posterior packing device. We have our nasal drug delivery systems at the ready to administer midazolam, metoclopramide, glucagon, naloxone and opiates if the need arises as well. ...Luanne Freer, MD - Medical Director of Everest Base camp, Medical Director Yellowstone N.P.

Photo - topical oxymetazoline plus lidocaine to treat epistaxis at Everest Base Camp (photo compliments of Luanne Freer, MD)
Treatment protocol
2020- I need to revise this protocol, you should use atomized tranexamic acid as first line - apply much like this but probably don't need the cotton ball - just atomize and pinch. Whether adding a little oxymetazoline or lidocaine is helpful is not clear. Usually no cautery is needed.
*Download this protocol as MS word file - (click here -0.55 Mb)
Download this protocol as a PDF file (click here)
Indications: To induce vasoconstriction and stop bleeding in patients with anterior epistaxis (worth a try to slow down posterior bleeds as well)
Basic epistaxis tray materials:
- Tissue for patient to blow nose
- Bowl to capture runoff blood
- Gloves and mask for provider
- Cotton balls
- Medication cup
- Oxymetazoline bottle
- Atomizer (or use the bottle to spray)
- Clamp for nose
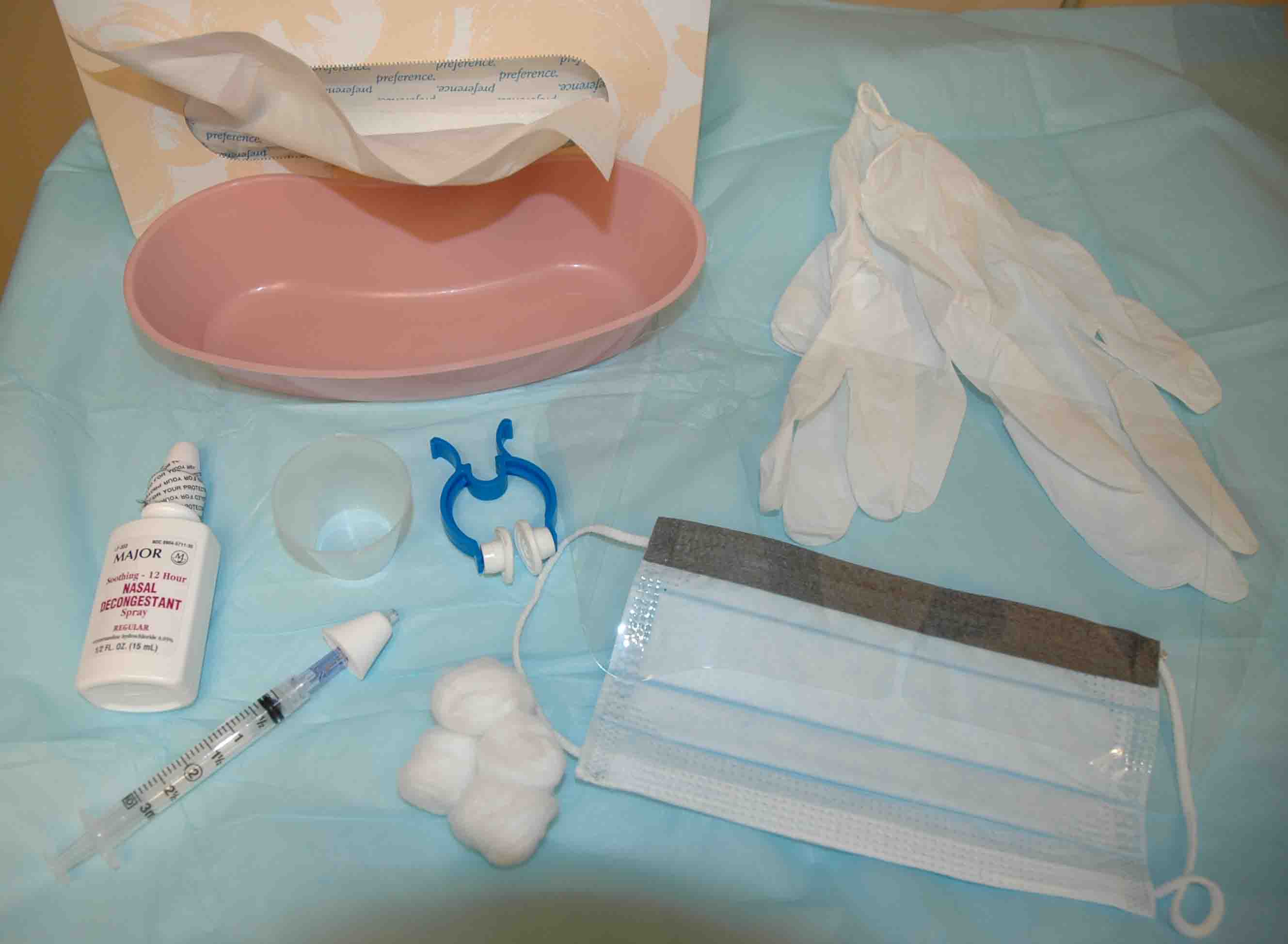
Preparation:
- Provide a gown, tray and tissue paper to the patient to capture the blood.
-
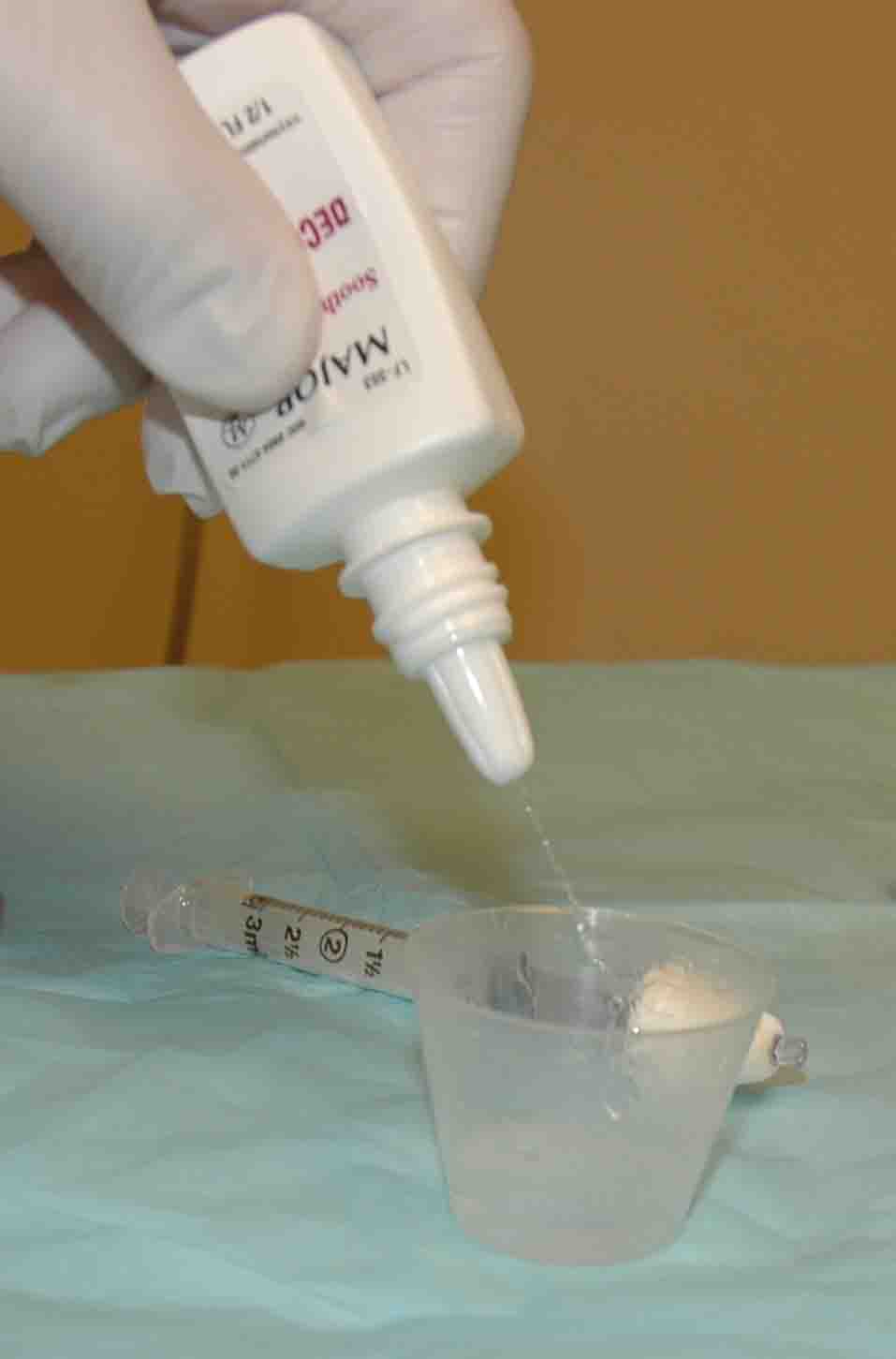 Squirt
oxymetazoline (Afrin) spray into a medication cup so it can be
easily drawn into a syringe.
Squirt
oxymetazoline (Afrin) spray into a medication cup so it can be
easily drawn into a syringe. -
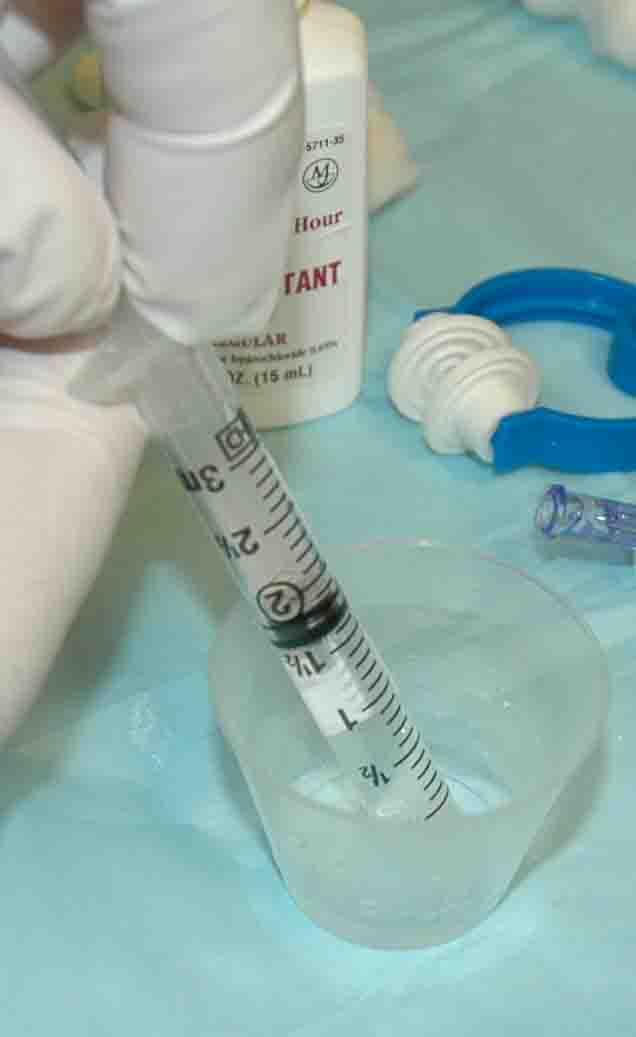 Draw
up 1.0 to 1.5 ml of oxymetazoline (Afrin) into a 3 cc syringe.
(Option - Also draw up 0.5 ml of 4% lidocaine into the same syringe
for anesthesia n case you need to use cautery).
Draw
up 1.0 to 1.5 ml of oxymetazoline (Afrin) into a 3 cc syringe.
(Option - Also draw up 0.5 ml of 4% lidocaine into the same syringe
for anesthesia n case you need to use cautery). - Connect the syringe to a syringe driven atomizer.
-
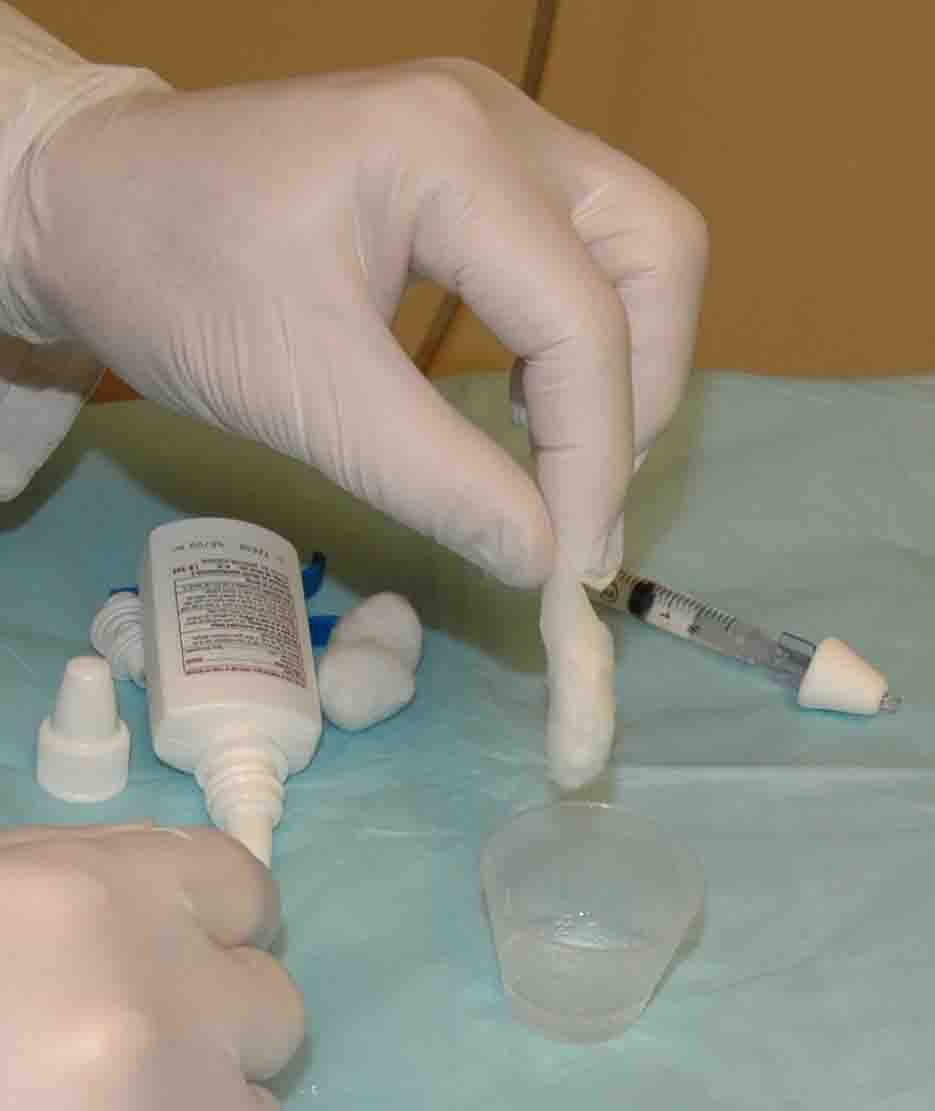 Put
a cotton ball in the remaining oxymetazoline and soak the cotton
ball. (double the dose and
use two cotton balls if both sides are bleeding)
Put
a cotton ball in the remaining oxymetazoline and soak the cotton
ball. (double the dose and
use two cotton balls if both sides are bleeding)
Procedure:
-
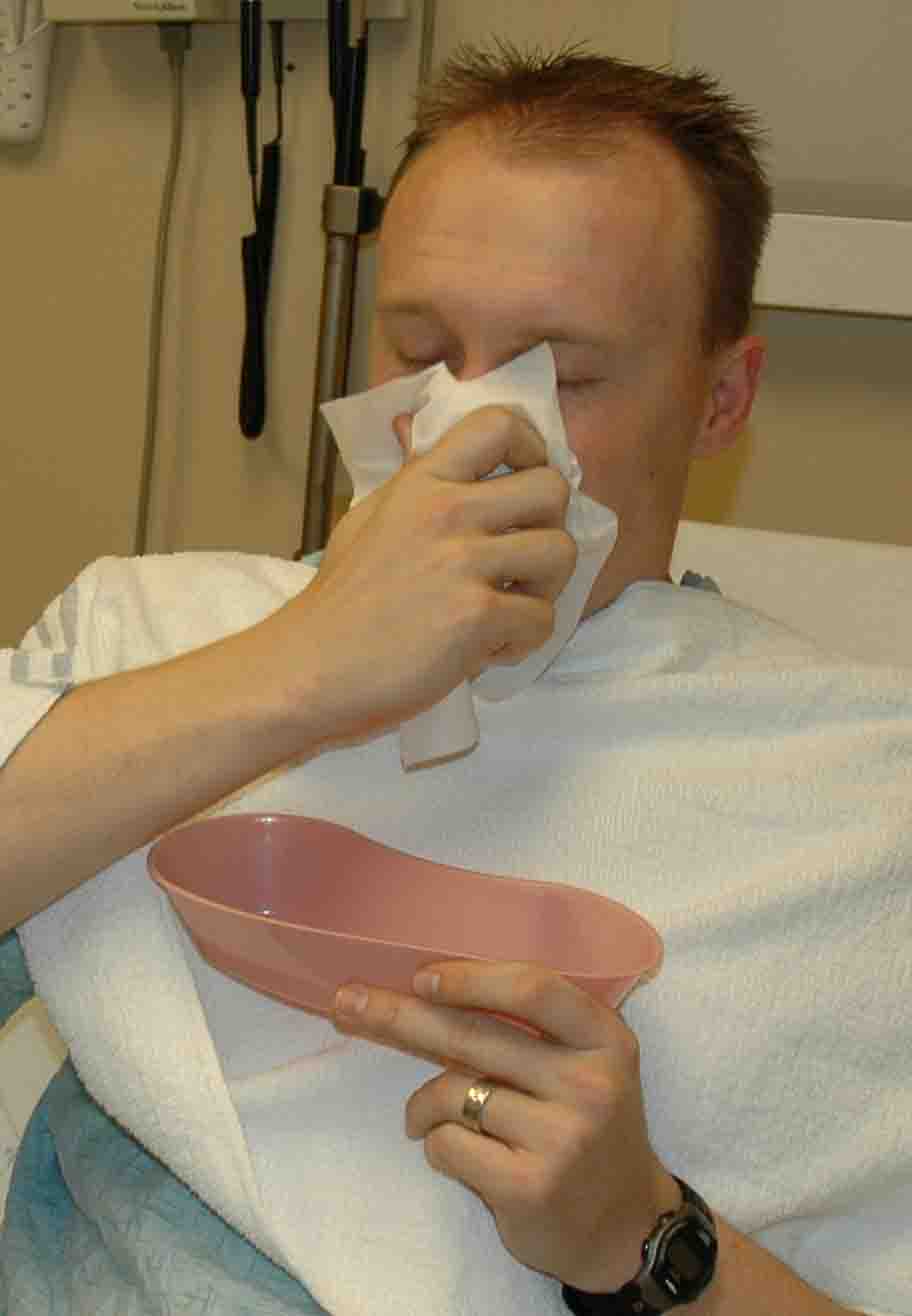 Ask
the patient to blow their nose to clear all the blood clots from the
nasal passage. This will clear the nasal cavity and expose the nasal
mucosa so the medication is more effective.
Ask
the patient to blow their nose to clear all the blood clots from the
nasal passage. This will clear the nasal cavity and expose the nasal
mucosa so the medication is more effective. - Position the patient approximately 45 degrees recumbent in the bed.
-
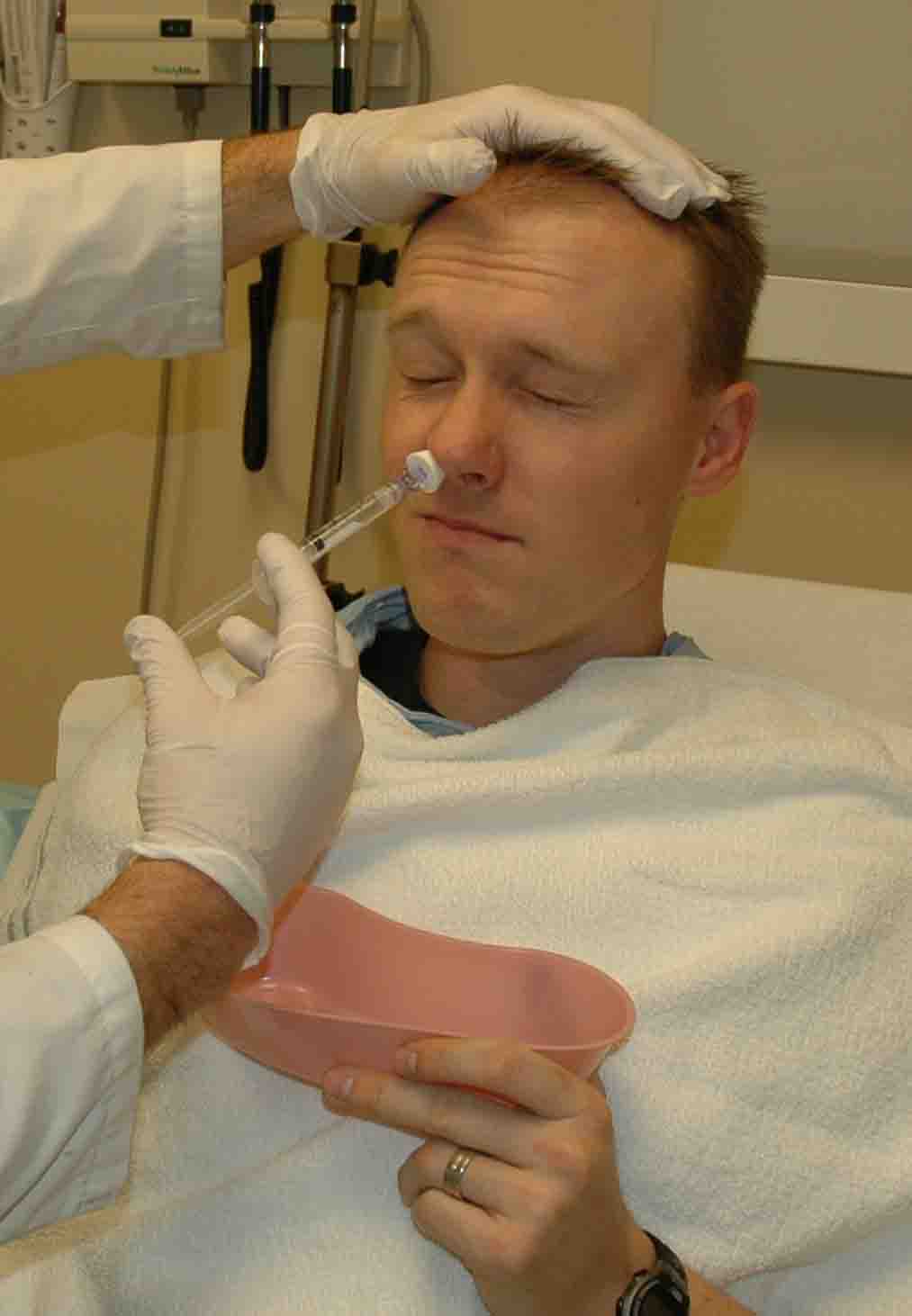 Place
atomizer within the affected nostril.
Place
atomizer within the affected nostril. - Briskly compress syringe to administer 1-1.5 ml of atomized spray into the affected nostril. Ask them to inhale through their nose during the time you spray.
- Allow the patient to capture any runoff blood and solution.
-
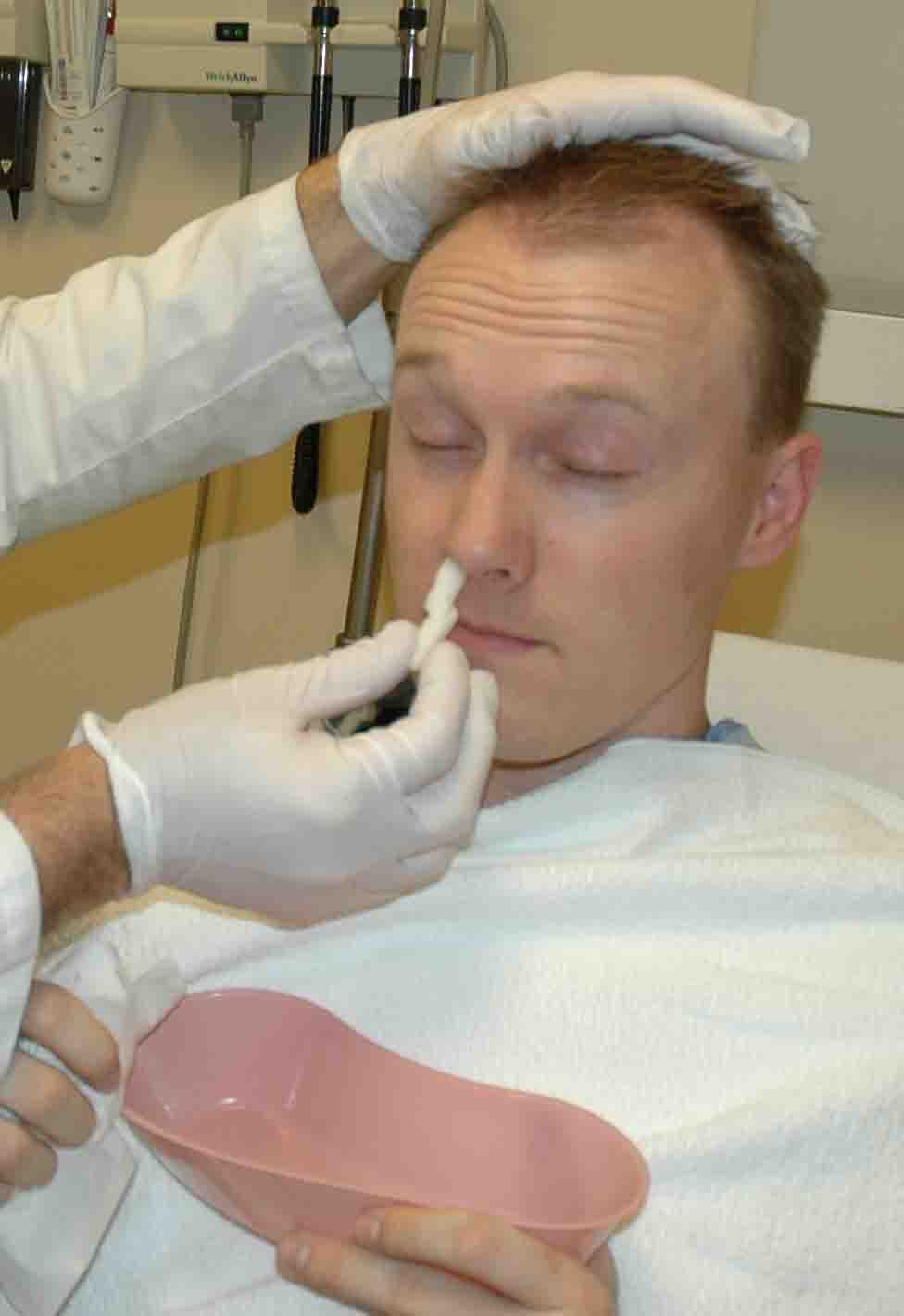 Take
the cotton ball soaked with oxymetazoline and roll into cigarette
shape. Place this into the
bleeding nostril.
Take
the cotton ball soaked with oxymetazoline and roll into cigarette
shape. Place this into the
bleeding nostril. - Repeat in other nostril if it is also bleeding.
- Tape a folded 4X4 across the nose to hold the cotton ball in place and capture blood.
- Sit the patient back up.
-
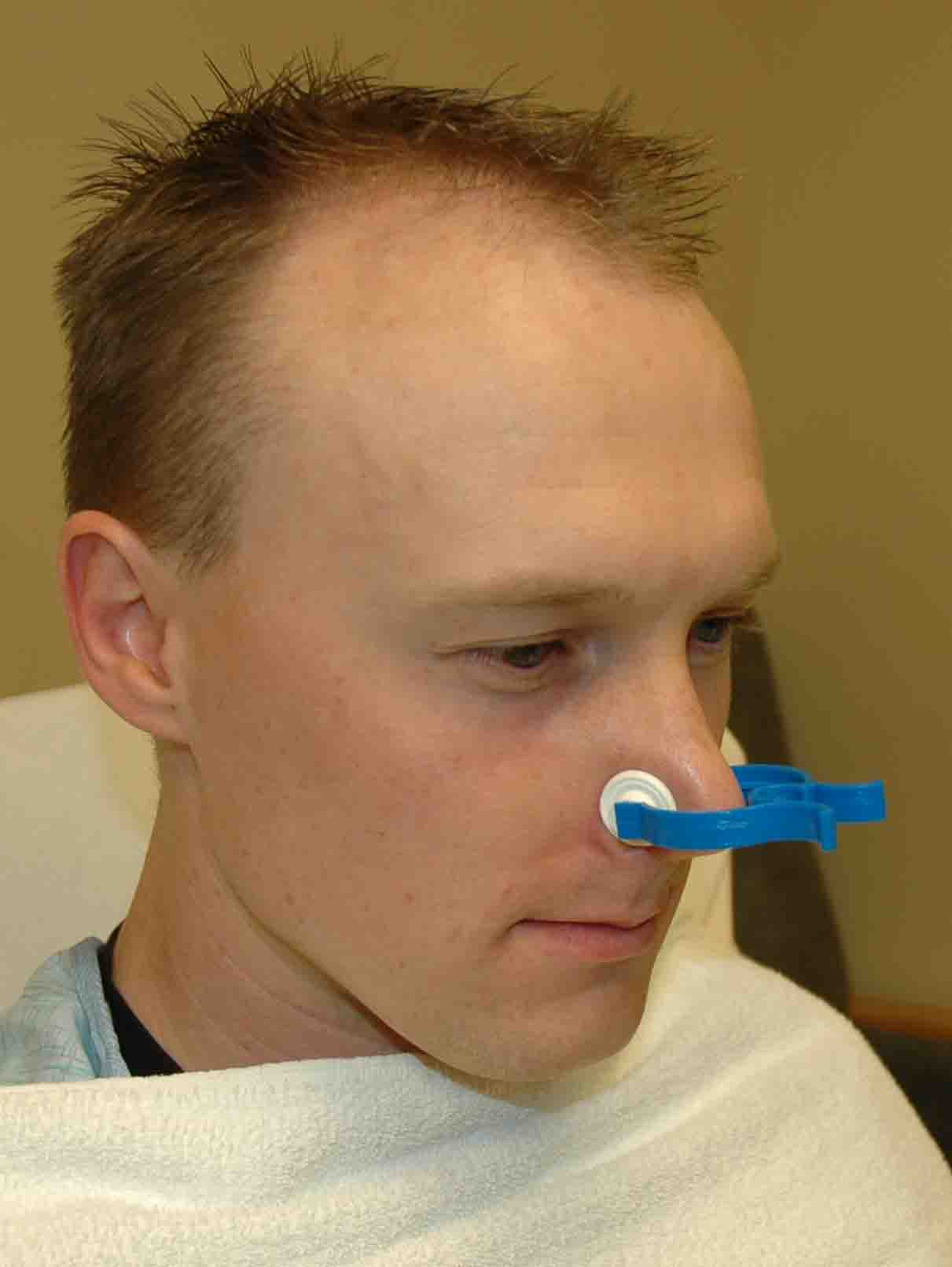 Ask
the patient to pinch their nostrils firmly with one hand to reduce
blood flow to the anterior nose. Alternatively you can clamp their
nose with a pre-made nasal clamp.
Ask
the patient to pinch their nostrils firmly with one hand to reduce
blood flow to the anterior nose. Alternatively you can clamp their
nose with a pre-made nasal clamp. - Wait 15 minutes.
-
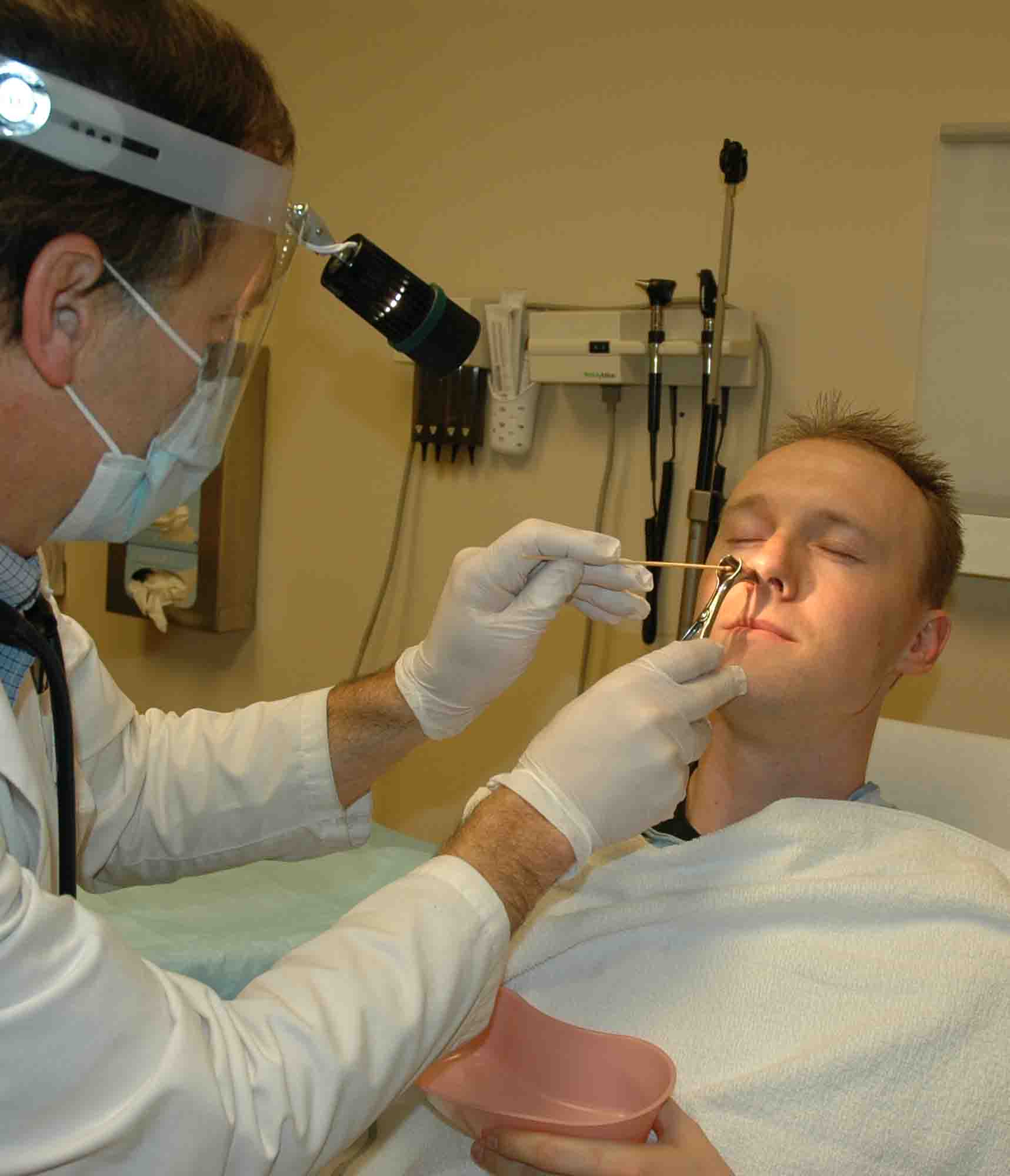 Return,
remove the gauze and packing, cauterize any anterior vessels that
require cautery (usually not needed).
Return,
remove the gauze and packing, cauterize any anterior vessels that
require cautery (usually not needed). - If bleeding persists obtain topical thrombin and repeat the above procedure using thrombin as the atomized spray and applying another cotton ball soaked in oxymetazoline - this gives clotting effect plus vasoconstriction.
- Discharge the patient with instructions to use oxymetazoline spray every 8 hours for the next 48-72 hours to maintain vasoconstriction. Forewarn them to not use the oxymetazoline for a longer period due to rebound edema problems. Instruct them to apply topical Vaseline or other appropriate material to the anterior nose twice a day to keep the mucous membrane from drying and cracking.
Download this protocol as a MS Word file - (click here 0.55 Mb)
Bibliography (click here for abstracts)
1. Evans, J.A. and T. Rothenhaus, Epistaxis. Emedicine, 2007: p. http://www.emedicine.com/EMERG/topic806.htm.
2. Bent, J.P., 3rd and B.P. Wood, Complications resulting from treatment of severe posterior epistaxis. J Laryngol Otol, 1999. 113(3):252-254
3. Monte, E.D., M.J. Belmont, and M.K. Wax, Management paradigms for posterior epistaxis: A comparison of costs and complications. Otolaryngol Head Neck Surg, 1999. 121(1): p.103-6
4. Hady, M.R., K.Z. Kodeira, and A.H. Nasef, The effect of nasal packing on arterial blood gases and acid-base balance and its clinical importance. J Laryngol Otol, 1983. 97(17): p. 599-604
5. Katz, R.I., et al., A comparison of cocaine, lidocaine with epinephrine, and oxymetazoline for prevention of epistaxis on nasotracheal intubation. J Clin Anesth, 1990. 2(1): p. 16-20
6. Lennox, P., et al., Local anaesthesia in flexible nasendoscopy. A comparison between cocaine and co-phenylcaine. J Laryngol Otol, 1996. 110(6): p. 540-2
7. Groudine, S.B., et al., New York State guidelines on the topical use of phenylephrine in the operating room. The Phenylephrine Advisory Committee. Anesthesiology, 2000. 92(3): p. 859-64.
8. Greher, M., et al., Hypertension and pulmonary edema associated with subconjunctival phenylephrine in a 2-month-old child during cataract extraction. Anesthesiology, 1998. 88(5): p.1394-6
9. Kalyanaraman, M., et al., Cardiopulmonary compromise after use of topical and submucosal alpha- agonists: possible added complication by the use of beta-blocker therapy. Otolaryngol Head Neck Surg, 1997. 117(1): p. 56-61.
10. O'Hanlon, J. and K.W. Harper, Epistaxis and nasotracheal intubation--prevention with vasoconstrictor spray. Ir J Med Sci, 1994. 163(2): p.58-60
11. Riegle, E.V., et al., Comparison of vasoconstrictors for functional endoscopic sinus surgery in children. Laryngoscope, 1992. 102(7): p.820-3
12. Doo, G. and D.S. Johnson, Oxymetazoline in the treatment of posterior epistaxis. Hawaii Med J, 1999. 58(8): p.210-12.
13. Krempl, G.A. and A.D. Noorily, Use of oxymetazoline in the management of epistaxis. Ann Otol Rhinol Laryngol, 1995. 104(9 Pt 1): p. 704-6.14. Chen, S. t., T. Karnezis, et al. (2011). "Safety of intranasal Bevacizumab (Avastin) treatment in patients with hereditary hemorrhagic telangiectasia-associated epistaxis." Laryngoscope 121(3): 644-646
15.
Heymer, J., T. Schilling, et al. (2018). "Use of a mucosal atomization
device for local application of tranexamic acid in epistaxis." Am J
Emerg Med 36(12): 2327.
16. Zahed, R., et al.,
A new and rapid method for epistaxis treatment using injectable form of
tranexamic acid topically: a randomized controlled trial. Am J Emerg
Med, 2013. 31(9): p. 1389-92.
 Therapeutic
Intranasal Drug Delivery
Therapeutic
Intranasal Drug Delivery